Reducing sitting time improves insulin sensitivity, 24-hour glucose levels, duration of hyperglycaemia and fasting triacylglycerol levels in adults with Type 2 diabetes.
Moderate to vigorous physical activity is one of the cornerstones in the prevention and treatment of Type 2 diabetes. Current physical activity guidelines recommend at least 150 min per week at these intensities. Despite the proven effectiveness, poor adherence to these guidelines is a major public health challenge. Non-compliance is likely to be even higher in those with type 2 diabetes, in which related comorbidities such as obesity and muscle weakness can be a barrier to physical activity. An alternative approach is needed.
A recently published study by Duvivier et al. (in scientific journal Diabetologia) demonstrated that reducing sitting time can have desirable effects for adults with Type 2 diabetes.
The Study
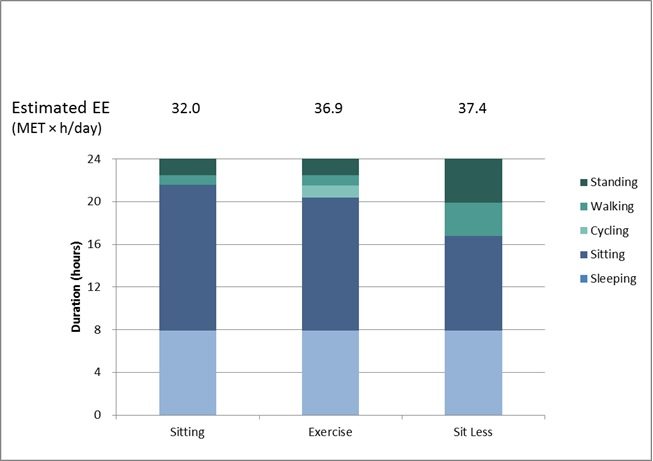
This study considered the possible benefits of a ‘sit less’ programme, replacing sitting time with standing and light-intensity walking, in comparison to the use of a conventional structured exercise regimen of the same energy expenditure. Nineteen adults (13 men and 6 women) with Type 2 diabetes with a mean age of 63 years and mean BMI of 30.5 kg/m2 participated in the randomised intervention study. All participants followed three activity regimens – ‘Sitting’, ‘Exercise’ and ‘Sit Less’ – each lasting 4 days, with 10 days between regimens.
- Sitting regimen: participants were restricted to 1 hour/day of walking and 1 hour/day standing, with the remaining 14 hours spent sitting.
- Exercise regimen: approximately 1 hour/day of sitting time was replaced by cycling.
- Sit Less regimen: 5 hours/day sitting were replaced by 2 hours walking and 3 hours standing.
Diet was controlled with use of pre-packed meals during each regimen. Glucose levels were measured continuously using a subcutaneous glucose monitor. Physical activity and sedentary behaviour was verified using 24-hour activity trackers (accelerometer). Glucose levels were analysed during the last 24 hours of each four-day regimen. On the day after each regimen, blood was collected for glucose, insulin and lipid measurements.
Results
The sit less regimen led to significant improvements in insulin sensitivity, 24-hour glucose levels, durations of hyperglycaemia and fasting triacylglycerol levels compared with sitting. Whilst positive effects for most variables were also found in the traditional exercise regimen, these were generally non-significant or less evident than the improvements found for the sit less group.
Conclusion
The outcome of the study fits the emerging picture that breaking up sedentary behaviour with light-intensity activities may be a potent way to help improve blood glucose control. Therefore apart from including exercise in our lifestyle, health advice should also focus on decreasing sedentary time and moving more on a daily basis. One of the strategies to monitor daily activity is the use of an activity tracker which can promote daily movements and physical activity. Physical activity trackers have gained popularity to assist individuals in monitoring their level of activity and reaching their daily activity goals.
Reference:
Duvivier, B.M.F.M., Schaper, N.C., Hesselink, M.K.C. et al. Diabetologia (2017) 60: 490.
Download the article here.
For more information about this study, please contact:

Bernard Duvivier, MD
Department of Human Movement Sciences
Maastricht University Medical Centre
Maastricht, The Netherlands